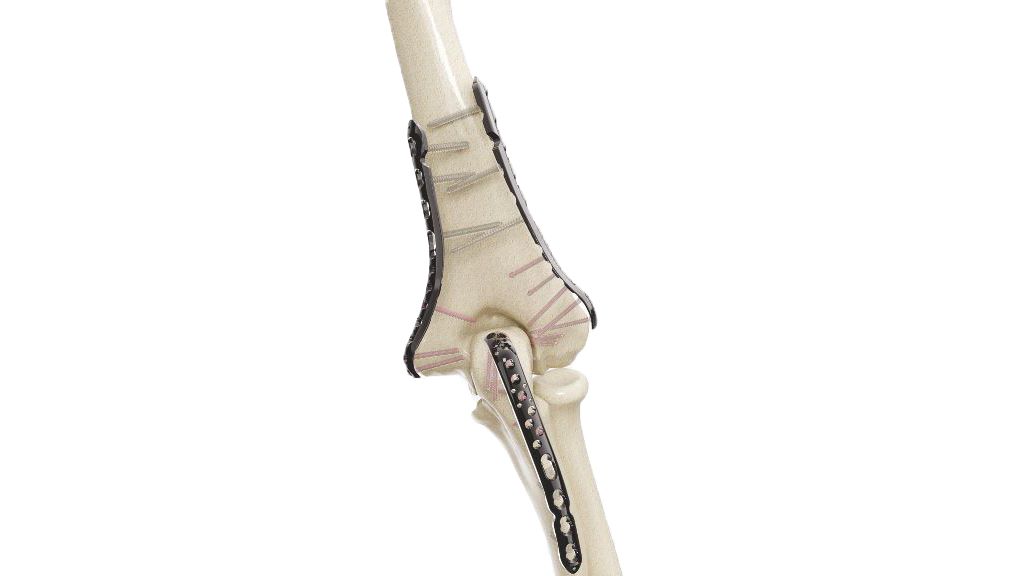
Distal Humerus Plate - Posterolateral Without Support (VALP)
Product Overview
The 2.7/3.5 Distal Humerus - Posterolateral Without Support Plates (VALP) is an orthopedic implant designed for fractures and reconstructive procedures involving the distal humerus. Its anatomical shape and precise construction allow for effective stabilization without the need for additional lateral support plates. With versatile screw options and anatomical contouring, it offers optimal fixation and promotes efficient healing of distal humerus fractures.









Product Uses
- Fractures : Management of distal humerus fractures, including intra-articular fractures, comminuted fractures, and fractures with bone loss.
- Osteotomies : Correction of deformities or malunions through surgical bone cuts near the distal humerus.
- Non-unions : Treatment of non-healing fractures or failed prior fixation attempts.
- Revision surgeries : Revision of failed or inadequate prior surgical procedures involving the distal humerus.
- Trauma : Management of traumatic injuries to the distal humerus, such as fractures resulting from accidents or falls.
- Reconstruction : Restoration of bone anatomy and alignment in cases of bone defects or deformities.
Product Specification
- Plate Thickness : Available in 2.7 mm and 3.5 mm options.
- Plate Length : Variable lengths to accommodate different patient anatomies and fracture patterns.
- Plate Design : Anatomically contoured for optimal fit and alignment with the distal humerus.
- Screw Options : Combination of 2.7 mm and 3.5 mm screw options for versatile fixation.
- Material : Typically made from biocompatible materials such as titanium alloy or stainless steel.
- Surface Treatment : May feature surface coatings or treatments to enhance biocompatibility and osseointegration.
- Sterility : Supplied sterile for single-use, ensuring patient safety.
Distal Humerus Plate - Posterolateral Without Support (VALP) Sizes
Comprehensive Guide for Distal Humerus Plate - Posterolateral Without Support (VALP)
- Patient Evaluation : Review the patient's medical history, allergies, medications, and any co-existing conditions. Conduct a thorough physical examination, focusing on the affected limb and adjacent joints.
- Imaging Studies : Obtain X-rays, CT scans, or MRI to assess the fracture pattern, bone quality, and soft tissue involvement. Use imaging to plan the surgical approach, select the appropriate implant size, and determine screw trajectory.
- Surgical Planning : Choose the appropriate size and type of VALP implant based on pre-operative imaging and surgical judgment. Plan the surgical approach, considering anatomical landmarks, soft tissue integrity, and neurovascular structures.
- Patient Education : Educate the patient about the procedure, expected outcomes, potential risks, and post-operative rehabilitation. Provide instructions regarding pre-operative fasting, medication management, and any other relevant pre-operative preparations.
- Patient Positioning : Position the patient supine on the operating table with the affected arm prepared and draped in a sterile manner. Consider the use of arm supports or traction devices to facilitate exposure and access to the surgical site.
- Surgical Approach : Perform a standard or modified lateral approach to the distal humerus, depending on the fracture pattern and surgical preference. Use meticulous dissection to expose the fracture site while protecting surrounding soft tissues and neurovascular structures.
- Fracture Reduction : Reduce the fracture fragments anatomically using manual manipulation, traction, or specialized reduction tools. Confirm reduction and alignment under fluoroscopy or intraoperative imaging guidance.
- Implant Placement : Prepare the bone surfaces and position the "2.7/3.5 Distal Humerus - Posterolateral Without Lateral Support Plates (VALP)" using appropriate instrumentation. Secure the plate to the bone using locking or non-locking screws, ensuring optimal fixation and stability.
- Closure : Irrigate the surgical site thoroughly to remove debris and reduce the risk of infection. Close the incision in layers using absorbable sutures for deeper tissues and non-absorbable sutures for skin closure.
- Immediate Post-Operative Period : Monitor the patient closely in the recovery room for signs of anesthesia recovery and immediate post-operative complications. Administer analgesics and antiemetics as needed to manage pain and nausea.
- Early Mobilization and Rehabilitation : Initiate early range of motion exercises as tolerated to prevent stiffness and promote joint mobility. Coordinate with physical therapy for a structured rehabilitation program tailored to the patient's specific needs and functional goals.
- Follow-Up and Monitoring : Schedule regular follow-up appointments to monitor healing, assess implant stability, and evaluate functional outcomes. Perform periodic X-rays or other imaging studies to assess fracture union, implant position, and any signs of complications.
- Activity Restrictions : Advise the patient on activity restrictions and precautions to prevent excessive stress on the healing bone and implant. Encourage compliance with prescribed rehabilitation protocols and restrictions to optimize recovery and minimize complications.









.png)